- within Immigration topic(s)
- with readers working within the Environment & Waste Management industries
Introduction
Research programs that are part of Academic Medical Centers (AMC) are uniquely positioned to accelerate the translation of research into clinical care. The central role of a clinician scientist in the AMC drives innovation from the viewpoint of health and disease. An organizational structure supporting basic, clinical and translational research creates a natural pipeline for innovation from fundamental biological discoveries to long-term health outcomes. Like many other factors affecting the healthcare system, artificial intelligence (AI) is fast becoming a significant disruptor to the traditional academic research model and more specifically, the translational research model which focuses on the translation of scientific discovery and innovation to clinical and health impact. This paper highlights some of the critical challenges that AMC-based research programs face and new opportunities presented, and introduces a framework outlining key steps AMCbased research organizations will need to take to prepare for AI and develop their programs.
Context: Unique Characteristics of an AMC-Based Research Organization
Unlike many commercial research organizations that have centralized, top-down structures for establishing research agendas and organizing resources, AMC-based programs are complex ecosystems that emphasize flexibility, creativity and accountability at an individual Principal Investigator (PI) or research faculty level. These organizations are often characterized by department-based and center/institute-based research programs that enable individual PI driven research efforts, with institutional support provided through shared infrastructure—administrative services such as grants management; scientific infrastructure including cores and lab space, and others—and program funding.
Researchers are often attracted to the AMC-based model because of the academic culture, collegial environment, opportunity to teach and the relative intellectual freedom through grant funding. AMC-based clinician scientists have dual professional incentives; direct patient care and research output measured by publications and achievement of a sustained, growing portfolio of sponsored research. Increasingly in AMC-based research programs, researchers may be rewarded for translation of their research products into patient care.
The primary vehicle driving translation is commercialization of their discoveries into intellectual property that can attract investment from third-party companies. The ultimate goal is to impact health by launching and sustaining academic research products in the marketplace. This differs from commercial research organizations whose sole focus is product development, and ultimately, financial value for company owners or public shareholders.
Another distinguishing feature of the academic research environment is that research programs are often carried out within healthcare delivery systems, enabling access to patients, providers and the care delivery revenue cycle. This integration creates opportunities to more readily develop and test innovations in the care setting and translate clinical research evidence into care models, speeding adoption and increasing impact. This opportunity carries with it an increased responsibility for managing risk and health system economics since unproven innovations can directly impact patient care and the financial performance of healthcare delivery systems.
AI Challenges in an AMC-Based Research Environment
AMC-based research organizations are faced with a range of AI-related challenges, some that are more generalized to the broader industry and some that are unique to their environment. The key challenges they face can be organized into the following six categories:
Culture and Resource Alignment
Research across a large AMC-based research organization is varied and often somewhat fragmented from the perspective of a traditional corporate culture. This is by design, as grant funded individual investigators create new knowledge based on academic incentives and are able to fund much of their work through independent grants and philanthropy. The incentives to align programs and individual researchers around emerging technological advances can be extremely challenging—particularly those that originate outside the traditional domains of biomedical research and are as transformative—and costly—as big data and AI. Historically, incentives for academic advancement and career growth emphasize individual achievement within the researcher's area of expertise (e.g., publications within the disease area e.g. oncology, grant funding) which fosters a culture of independence and beneficial competition.
Grants, as the primary funding source for PIs, provide focus and priority. AI requires an intellectual approach that is multi-disciplinary, bringing together traditional biomedical and clinical research experts with artificial intelligence experts, computer scientists, data scientists, informaticists, implementation scientists and multiple care provider areas, including nursing and advanced practice providers. Successful AI initiatives within the academic research environment will need to evolve incentives to reward team science and publication outside of traditional academic journals, develop new mechanisms to attract computational, mathematics and highperformance computing experts from across the different disciplines in a collaborative model that appreciates their individual interests while creating shared incentives and collective benefit.
Additionally, although the academic environment includes a broad range of skills, it is unlikely that any one academic institution has the breadth and depth of resources necessary to discover and translate AIbased innovation into applications that impact successful AI initiatives will need to include partnerships with commercial vendors and other academic institutions, in particular to access computer science and engineering talent.
Governance
Generative AI platforms are highly complex and are designed to evolve, making them difficult to predict and manage. Introducing generative AI innovations into the clinical environment carries significant responsibility and requires new approaches to objectively measure and evaluate performance against known benchmarks. Most AMC-based research organizations have the benefit of access to clinical environments—and the patient populations and rich data that comes with them—and, as a result, share in this responsibility to manage the risks introduced by research innovation. Additionally, the AI regulatory environment is immature and rapidly evolving. AI programs will need to monitor new regulations and be prepared to respond as changes are made.
Although AMC-based research organizations have well-established governance structures and processes including Institutional Review Boards (IRBs), these will likely be insufficient in their scope of oversight and influence and the depth of expertise represented by their members. AI will require new cross-enterprise governance structures that integrate the clinical system and research oversight models and can address complex issues including defining AI performance evaluation, risk management criteria, partnership strategy and contracting, data privacy, access and use policies and prioritization of resources across the research and clinical care domains.
Leadership and Accountability
Related to the governance challenges, AI programs will require changes to the AMC-based research organizational structure. AI-related research initiatives are growing organically across AMC-based research organizations and have insufficient coordination, support and oversight. Establishing dedicated AI leadership to promote innovation, and develop standards, shared infrastructure and optimize use of computational resources, is critical. Additionally, within the AMC structure, clinical system leaders are prioritizing and advancing AI programs focused on operational and clinical use cases. Enhanced coordination across the clinical and research domains will be necessary to maximize the unique skill sets of researchers, clinical system data and shared infrastructure. It will be critical to establish shared priorities and first principles for governing AI so that the creative potential of the research domain can be realized. Without a dedicated research AI leader who can represent research interests and serve as a single point of coordination, organizations run the risk of having bifurcated AI programs that underserve the interests of the clinical and research communities.
Funding
AI represents a transformative opportunity for organizations that are able to move quickly to build and maintain necessary skills and infrastructure. Costs for this are substantial, and accessing initial and sustained funding within a predominantly grantdriven financial model, at the pace of change created by emerging AI technologies, is difficult. Finding new funding sources either from the health system or through philanthropy will be necessary for those AMCs that aspire to drive innovation.
Funding Challenges for Research Programs at AMCs
A promising generative AI study at the Children's Hospital of Philadelphia is estimated to require over $500,000 in compute time for only one of many experiments planned for the research study.
Rapid Cycle Time for New AI Technologies at Odds With Grant Cycles
The Current cycle time for game-changing AI innovation is significantly less than the typical three-tofive-year grant lifecycle. The release of major new foundation models such as Meta's Llama in 2023 greatly accelerated the pace of innovation. Pretrained foundation models that are generally available from companies such as Microsoft, Meta, Google and Amazon are opening up entirely new areas of research for those AMCs that are positioned to take advantage of them.
Scale
No single health system or AMCbased research organization has sufficient data for a large scale, truly transformative AI program. Additionally, the scale of computing resources necessary for the most innovative, high impact and valuable AI research far outstrips what is feasible for a typical AMC to acquire. Peer partnerships, data consortia and computing co-operatives will need to be formed. Additionally, advancements in Large Language Models (LLM), Natural Language Processing (NLP) and other AI-related technology is happening at increasing speed across the industry. Accessing industry expertise and advanced technologies to supplement AMCbased capabilities will be critical.
Scale Challenges for AMCs—Examples From the Field
Data: The Children's Hospital of Philadelphia has fewer than 200,000,000 pages of clinical documentation that could be used for important AI research. Comparatively, the now-obsolete GPT3 model from OpenAI is estimated to have been trained on more than 600,000,000 pages.
Computing Resources: Harvard's Kempner Institute purchased 384 state of the art graphical processing units at an estimated cost of $15,000,000 in hardware alone. This was an upgrade from the 144 prior-generation GPUs purchased only two years earlier.
Speed
AI is a highly competitive field. Academic research organizations are competing with peers, some who are much larger and have greater access to resources, and industry, who is well funded and designed for scale and speed. To be effective, academic research AI programs will require prioritization and a clear vision that defines a focused role within the broader AI industry allowing the program to narrow its strategies and be more targeted in investing limited resources. It will also be needed to inform their recruitment and partnership strategies.
Amid sweeping declines in venture activity, funding to AI startups remained resilient in 2023, falling just 10% YoY to $42.5B. One-third of this ($14B) was raised by just three companies—OpenAI, Anthropic and Inflection—as the race to develop more advanced LLMs heats up.
Feb. 1, 2024. State of AI 2023 Report, CB Insights Research.
AI Opportunities in an AMC-Based Research
Although the complexities and barriers are significant, the potential for AI to be a transformative force in clinical and translational research is compelling. The potential opportunities fit into two broad categories:
AI as an enabler of research:
- Using AI to reduce or eliminate timeconsuming mundane activities and thereby improve the speed and efficiency of the research. Examples include large data set acquisition and preparation, identification of peer studies and results, etc.
- Using AI as a tool to simulate clinical trials and allow PIs to model variables including inclusion criteria to test and optimize their models before initiating the trial. The benefits include improved precision and increased patient enrollment.
- Using AI as a tool to generate synthetic patients and rapidly test hypotheses in a no-risk environment before moving ahead with a clinical trial. The benefits include lower patient risk, improved precision and increased likelihood of successful trials.
AI as an Enabler of Research: Case Example
A study published by researchers at The Children's Hospital of Philadelphia used AI to learn a normal pattern of growth for children's brains, similar to a pediatrician's growth chart. (LINK)
Development of novel AI-based capabilities:
- Ability to scale human expertise. Using AI to augment the work
of scarce medical experts could result in improved patient outcomes
and a more accessible and equitable health system. For example,
augmented intelligence capabilities could help deliver:
- Faster, higher quality results to improve outcomes by decreasing timetotreatment (e.g., point of care clinical decision support; diagnostics and imaging—augmented lung and breast imaging).
- Extending access to high quality of care creating a more consistent and equitable healthcare delivery system.
- Creating efficiencies that reduce or eliminate unnecessary cost and manual effort (e.g., autonomous AI-based medical coding to reduce manual coding volume, cost and time while improving efficiency and accuracy; use of AI simulation to facilitate/augment medical training; creation of synthetic research datasets to overcome data privacy/use and volume issues and the time required to access and organize research data).
Scaling Human Expertise: Case Example
Medtronic's Gi Genius(tm) AI-based Computer Aided Polyp Detection system helps gastroenterologists in real time to increase their adenoma polyp detection rates by 14% as demonstrated in a randomized controlled trial. (LINK)
Framework for AI Within an Academic Research Environment
AMC-based research organizations have limited resources. It's critical that they have a clear understanding of what their capabilities are, how AI can align with their broader strategic goals and imperatives and what role they want to have in the AI industry.
There are three general approaches worth consideration. Most AMC-based research organizations will have a portfolio of AI initiatives that span these approaches and will need to determine how they want to balance investments to support each:
- Productivity: Focus on AI-driven automation to streamline common research functions that are time consuming (e.g., AI-enabled clinical trials, data extraction and organization, identification of similar studies and access to their related publications, etc.). This approach may provide limited commercial opportunity but broad benefit to the research staff. There are fewer challenges with these opportunities as they would have less direct impact on clinical care and can be organized and delivered as part of a research organization's infrastructure support. This is likely a combination of "buy and build" strategies.
- Destination clearinghouse for new AI technology adoption: Create a platform to test new AI-based solutions within the healthcare environment and/or modify new technology for adoption within the health system. Again, there may be modest commercialization opportunity, but this approach could help maximize an organization's ability to leverage new AI innovations and limit adoption risk. The platform would likely require partnerships with peer institutions or others who can help provide sufficient data to support broad use cases and close collaboration between the research and clinical care organizations to facilitate and oversee translation into the care models. This is a "buy and modify" strategy
- Creator: Become an incubator for novel AI innovations. Although the most complex and challenging approach, it creates the greatest opportunity for industry impact and commercialization. This would require industry partnerships and significant governance to manage risk. This is a "build" strategy.
Planning Roadmap
Each organization will start from a different place but may want to consider the following six steps in organizing their AI program and developing their AI strategy:
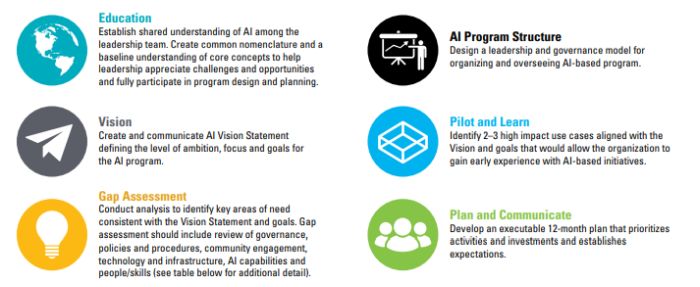
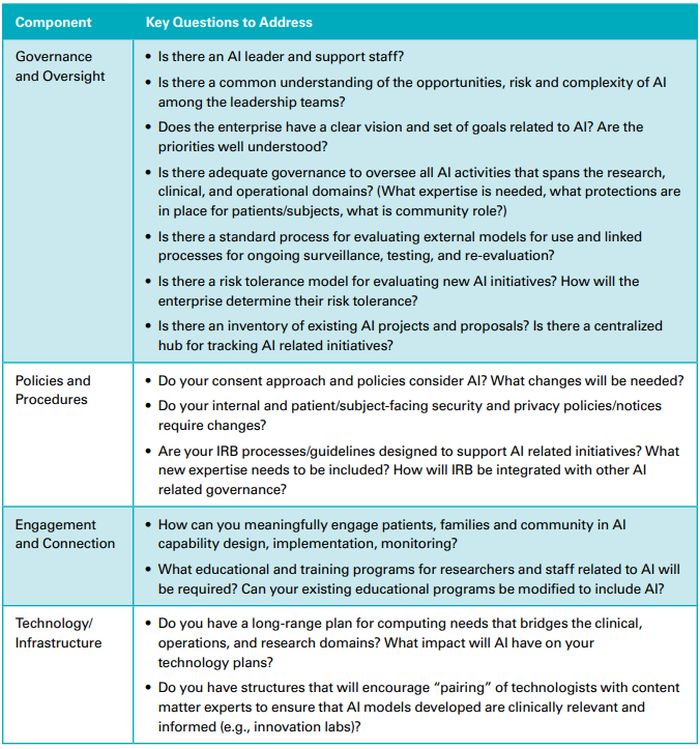
The following table provides a structured model for assessing AI readiness and organizing AI program planning. Organizations may want to prioritize development of different aspects of their AI programs based on how they respond to the following questions:

Conclusions
Imagine a future where AI can help providers deliver better care to patients in the most resourceconstrained health systems. Over 1,300 Critical Access Hospitals (CAHs) provide front line care to rural communities in our country. By law, these hospitals only receive supplemental funding if they limit lengths of stay to 96 hours, have fewer than 25 patient beds and provide 24/7 emergency department care. These conditions require them to operate under extreme financial constraints. Advanced Practice Providers such as physician assistants, nurse practitioners and clinical nurse specialists often provide direct service to patients. AI has the potential to extend the ability of these skilled professionals to perform advanced health screening, provide a broader range of diagnostic services, access critical clinical expertise when needed and offer aspects of specialty and acute care otherwise unavailable to these communities. AMCs are uniquely positioned not only to teach medical students but also teach AI systems to bring the cutting edge expertise of their care providers to the dedicated professionals working hard to improve the health of patients at CAHs, public hospitals and beyond.
Using AI to create needed efficiencies for our providers and AMC-based research organizations, help lower costs, and to improve access, consistency and quality of care, will result in a more equitable and sustainable system of care. There are many challenges to organize, fund and manage effective AI programs in an AMC environment, but the potential rewards are great and the risks of missed opportunity and declining viability associated with inaction are compelling.
The content of this article is intended to provide a general guide to the subject matter. Specialist advice should be sought about your specific circumstances.
[View Source]


